Emergency Management
Cases of dentoalveolar trauma in general dental practice are relatively common. Catherine Coyle gives her advice on best practice
Traumatic dental injuries are a relatively common occurrence, with 13 per cent of children in the United Kingdom reportedly experiencing trauma to their permanent incisor teeth by age 15 (Child Dental Health Survey, 2003).
Thus the likelihood of children and adolescents presenting to their general dental practitioner for emergency management is high. Timely and appropriate intervention at this early stage can lead to significantly improved intermediate and long-term clinical outcomes for the patient.
Guidelines for management of dental injuries
The International Association of Dental Traumatology (IADT) and the British Society of Paediatric Dentistry (BSPD) informs dental practitioners of the current guidelines in initial management of dentoalveolar trauma. IADT guidelines are available at http://www.iadt-dentaltrauma.org while the BSPD guidelines are available from http://www.bspd.co.uk
Optimal treatment of intruded and avulsed teeth is controversial, with variation between guidelines. Hence the reader is directed to the above websites for further reading on the subject.
Facial bone fractures are uncommon in children and their management is beyond the scope of this article. Maxillofacial trauma is described elsewhere in the literature.
History of the injury
A thorough history and examination of the patient at the outset is mandatory. Whenever possible, photographs should form part of the patients’ records. Increasingly, dental injuries have the potential to become the subject of insurance claims or litigation, hence the dentist should be always be mindful of the particular importance of comprehensive, accurate and contemporaneous note taking.
The history should elicit the following information:
- When did the trauma occur? The interval between injury and treatment influences the prognosis. A delay in seeking help may raise suspicion of non-accidental injury (NAI)
- Where did the trauma occur? May indicate if tetanus prophylaxis is needed
- How did the trauma occur? Can elicit information on the type of injury to be expected. Any inconsistency between history and clinical findings may raise suspicion of NAI
- Who was present? Can yield further information on the nature of the accident and the presence of other injuries
- Were there any other injuries? These may take precedence over dental injuries
- Are there any lost teeth or fragments? Clarifies if a chest or soft tissue radiograph is indicated
- Previous medical history? Severe immunosupression, bleeding disorders, congenital heart disease, allergy to penicillin may influence treatment plans
- Previous dental history including any dental trauma? Provides insight into likely compliance for treatment and alerts to pre-existing compromised pulpal/periodontal status
- State of eruption of the teeth? Aids estimation of normal tooth position and root development
- What initial treatment has been given? Elicits the method of storage of teeth/ fragments, dry and wet times and replantations, if any, completed
- Is the patient up to date with immunisations? Determines the need for tetanus booster.
Examination
Full examination of the head and neck should be undertaken in a systematic and logical order, beginning extra-orally and recording visually or diagrammatically the position, size, shape and nature of any injuries. Intra-orally, the soft tissue status is recorded before examination of the hard tissues and teeth.
It is necessary to cleanse the area from any debris and crusted blood that is present with sterile saline and swabs, prior to attempting inspection of injuries. This serves the dual purpose of not only aiding visualisation of wounds, but also reassurance for accompanying parents that the injury may not be quite as severe as anticipated.
Urgent referral for medical assessment is indicated if there is evidence of any of the following:
- loss of consciousness, amnesia, vomiting, disorientation, speech difficulties, altered vision or unilateral dilated pupil; suggestive of head injury bruising behind the ears (Battle’s sign); suggestive of base of skull fracture
- bleeding from ears; suggestive of TMJ fracture
- fluid from nose/ears; suggestive of breach of dura mater.
In the absence of bodily injuries that take precedence over orofacial injuries, the following method of examination is suggested:
Extra-oral
- Soft-tissue wounds
- palpation of the facial skeleton to detect step deformities or tenderness
- assessment of cranial nerves – most notably VII (facial); the muscles of facial expression and V (trigeminal); the muscles of mastication.
Intra-oral
- Injuries to the oral mucosa and gingivae; check for missing tooth fragments embedded in deep wounds
- swelling; sublingual haematoma can occur in fractures of the mandible. Severely intruded maxillary teeth can present as a ‘bulge’ superior to the normal anatomical position of the tooth
- palpation of the alveolus; mobility or a step is suggestive of mandibular or maxillary fracture
- abnormalities of the occlusion; an anterior open bite is evident in bilateral condylar fractures. A lateral open bite in the contra-lateral side is present in unilateral condylar fractures
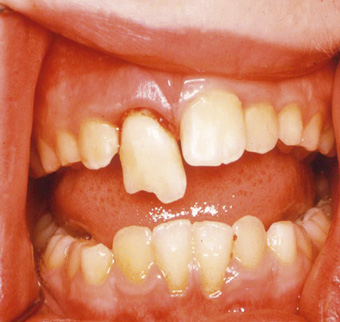
- displacement of teeth; luxations, extrusions (Fig 1), intrusions (Fig 2), avulsions, dentoalveolar fractures
- presence and extent of tooth fractures; pulp exposure (Fig 3), changes in colour, infractions
- mobility of teeth to digital pressure
- reaction to sensibility tests and percussion note; a high note is indicative of intrusion whilst a dull note may suggest subluxation or extrusion of a tooth. At the initial assessment post trauma, digital pressure is sufficient for determining tenderness to percussion (TTP).
Investigations: pulp sensibility testing
Sensibility testing may not be practical or reliable at the initial presentation. Nonetheless, tests provide an essential baseline measure of pulpal status. Responses to cold stimuli (ethyl chloride spray) should be recorded. The value of electric pulp testing in the emergency setting is equivocal.
Radiographs
Baseline radiographs are essential in both the initial management and the subsequent follow-up of traumatised teeth. Appropriate radiographs will facilitate diagnosis of injuries to the root and periodontal tissues and also assessment of the stage of root development.
When taking periapical films, it is preferable that several angles are taken for each traumatised tooth to determine the presence of root fractures and the direction of displacement of the root of the tooth.
The following radiographs could be taken, as dictated by nature of trauma, age of patient and number of teeth affected:
- two periapical films taken at angles to the arch
- upper oblique occlusal
- upper or lower anterior occlusal (particularly for young children)
- true lateral for intrusive luxations of primary anterior teeth
- lower occlusal with soft tissue contrast if a laceration to lower lip is present and tooth fragments are unaccounted for (Fig 4)
- referral for chest X-ray if teeth/fragments are unaccounted for and if respiratory symptoms have not been excluded.
Emergency treatment
In the case of primary tooth trauma, the presence of developing permanent successors and the likelihood that such patients will be pre-co-operative, determines how such injuries are managed.
For all dentoalveolar injuries, the following is recommended:
- pain relief
- soft diet for two weeks
- chlorhexidine mouthwash/chlorhexidine gel with gauze/cotton buds to use twice daily for one week
- use of soft toothbrush
- rigorous reinforcement of the need for good toothbrushing.
Composite and wire is the most commonly used splint (Fig 5). However, orthodontic brackets and wire has the advantage of allowing some gentle reduction of the injury. More recently, the titanium trauma splint has been advocated, which is significantly more user-friendly than traditional materials (Fig 6).
Soft tissue injuries
Typical injuries to the skin, oral mucosa and gingivae, are as follows:
Contusions
Contusions, or bruises not accompanied by a break in the mucosa, are often present without any dental injury and usually cause inconsequential submucosal haemorrhage. It is prudent, however, in the presence of an extra-oral contusion, to check the depths of the sulci for any deep wounds or degloving injuries.
Abrasions
Abrasions are superficial wounds caused by rubbing or scraping the skin or mucosal surface and commonly present on the lips, anterior gingivae, nose, forehead and chin (Fig 7). It is important that wounds contaminated with gravel or dirt are thoroughly debrided at initial presentation to avoid permanent tattooing.
Under local anaesthetic, the area requires copious irrigation with saline and/or chlorhexidine and scrubbing with gauze, a sterile brush or toothbrush. A scalpel blade can be utilised to scrape away any embedded foreign bodies within the wound.
Lacerations
Lacerations are wounds resulting from a tear. Gaping or ragged lacerations, or those which bleed persistently, will require suturing. Following debridement, skin wounds should be closed with a fine monofilament such as 6/0 Ethilon and only be performed by those who are competent to do so. Lacerations which cross the vermillion border are particularly important to approximate carefully, to avoid a step deformity of the lip and this should be the first part of the tissue to be repositioned and sutured.
Deep lip and cheek lacerations should be checked for tooth fragments before closure. When the lip has been bitten, typically by the upper teeth when they are intruded, it is imperative to check for through and through lacerations, which normally require closure in three layers: the muscle, the mucosa and the skin.
Skin sutures which are non-resorbable, should be removed four to five days later.
Extensive soft-tissue injuries should be referred elsewhere for appropriate management, for instance the nearest maxillofacial unit, via the local accident and emergency department arrangements.
Children presenting with contaminated wounds should be prescribed a broad-spectrum antibiotic such as Amoxicillin (in non-allergic patients).
Degloving injuries
Degloving injuries, in which a full thickness muco- periosteal flap is stripped off the bone, commonly result from blunt trauma. The detachment of gingivae can occur at either the dentogingival or the mucogingival junction (Fig 8).
The wound requires tight suturing to prevent the pooling of blood in the submental region, which could otherwise pose a risk to the patency of the airway.
Follow up of emergency treatment for trauma
While recommended protocols for follow-up of traumatised teeth vary according to the type of injury sustained, as a general guide, clinical and radiographic review is advised at one month, three months, six months and annually thereafter for five years, from the date of the initial trauma.
Close monitoring allows for early detection of loss of vitality and/or resorption, thus improving the likelihood of early intervention with a subsequent improved prognosis.
It is accepted that following initial emergency management of the patient, the general dental practitioner may wish for the patients’ care to be completed in the specialist paediatric setting.
Nevertheless, the role of appropriate and timely treatment at the outset, in limiting unfavourable sequelae and poor long-term outcomes, cannot be overemphasised.
Recommended guidelines for the treatment of injuries to hard and soft tissue, as well as primary dentition can be found by visiting http://bit.ly/IDMag-emergency-management
Irelands Dental Magazine
Table 1. Injuries to the hard tissues in permanent teeth
| Injury | Treatment |
|---|---|
| Enamel (uncomplicated)crown fracture | Adhesive build up or rebond fragment |
| Enamel-dentine (uncomplicated) crown fracture | Adhesive build up or rebond fragment |
| Enamel-dentine-pulp (complicated) crown fracture | Open apex/immature tooth
Open apex/immature tooth
Complete apex or non-vital tooth
|
| Crown-root fracture
(Enamel, dentine, cementum +/- pulp) |
|
| Root fracture
(cementum, dentine, pulp; may occur in the apical, middle or coronal third levels) |
|
| Dentoalveolar fracture
(alveolar bone; may involve the tooth sockets) |
|
Table 2. Injuries to the supporting tissues
| Injury | Treatment |
|---|---|
| Concussion
Tooth is TTP. No displacement. No radiographic abnormalities. |
|
| Subluxation
tooth is TTP with increased mobility but no displacement. Occasionally slight widening of the periodontal ligament (PDL) radiographically. |
|
| Extrusion
Tooth is displaced axially from socket. Occlusion often disturbed. Radiographically , the tooth appears elongated with an increased apical PDL space. |
Open apex/immature tooth
|
| Lateral luxation
Displacement other than axially with comminution or fracture of the alveolar socket. Radiographically, PDL space may be partly obliterated. |
|
| Intrusion
Displacement axially into the alveolar bone with comminution or fracture of the alveolar socket. Radiographically, PDL space absent from all or most of the root. |
Open apex
Closed apex
|
| Avulsion
Complete displacement of tooth from socket |
Tooth already re-implanted at presentation
Extra-oral dry time < 60minutes. Kept in milk, saline, saliva
Extra-oral dry time > 60minutes
|
Table 3. Injuries to the primary dentition
| Injury | Treatment |
|---|---|
| Uncomplicated crown fracture | Smooth off sharp edges or place adhesive restoration |
| Complicated crown fracture | Extract. Occasionally if compliance is good, pulpotomy may be possible. |
| Crown-root fracture | Extract. |
| Root fracture | No little mobility; manage conservatively Extract coronal fragment if displaced or mobile Allow apical portion to resorb |
| Alveolar fracture | GA may be required to reposition teeth and splint Monitor teeth in fracture line |
| Concussion | Conservative. Reassurance. |
| Subluxation | If very mobile and/or causing occlusal interference; extract Otherwise, conservative |
| Lateral luxation | If displacement is minimal, the tooth can be selectively ground out of occlusion. Otherwise, as above. |
| Intrusion | Allow spontaneous re-eruption. If apex is displaced palatally/towards developing tooth germ, extract |
| Avulsion | Do not replant |